Introduction
Whether you are prepping surgical instruments for a routine procedure, isolating a pathogen from a clinical sample, or just setting up a fresh batch of culture media, there is one rule that cannot be broken: your environment must be sterile.
In microbiology, sterilization isn't just a buzzword for "really clean." It is an absolute term. It refers to the complete destruction or physical removal of all forms of microbial life, including vegetative cells, fungi, viruses, and those stubbornly resistant bacterial endospores.
While sanitizers and disinfectants are great for reducing microbial loads on clinic countertops, they don't achieve true sterility. An item is either sterile, or it isn't.
Let's break down the essential methods used to achieve this gold standard.
What is Sterilization?
Sterilization is any process that removes or kills all forms of microbial life, including bacteria, viruses, fungi, and unicellular eukaryotic organisms. Sterilization is achieved when it removes a millionfold (10⁶) reduction of the most resistant spores. It is an important aspect in many fields, ranging from food production to medical fields. It is done using methods like heat, chemicals, or radiation, ensuring zero life expectancy after the procedure. After complete sterilization the surface is considered sterile and aseptic.
Sterilisation Vs. Disinfection

Importance of Sterilization
Sterilization is very important because it helps prevent infections, especially in medical settings like hospitals or during surgeries. By completely sterilizing instruments and surfaces, we reduce the risk of hospital-acquired infections and cross-contamination, hence improving outcomes. It is important in every field where microbial control is crucial.
Physical Methods of Sterilization
Autoclave or Steam Sterilization

An autoclave works on the principle of moist heat sterilization. It consists of a metal chamber filled with water, which upon exposure to high pressure of 15 psi or 775mm of Hg for 30mins, and this increases the temperature up to 121°C. This steamed vapor rapidly penetrates into deeper parts and helps eliminate the microbes and spores. After the completion of sterilization, the pressure is released through a whistle, and the pressure is restored back to ambient pressure.
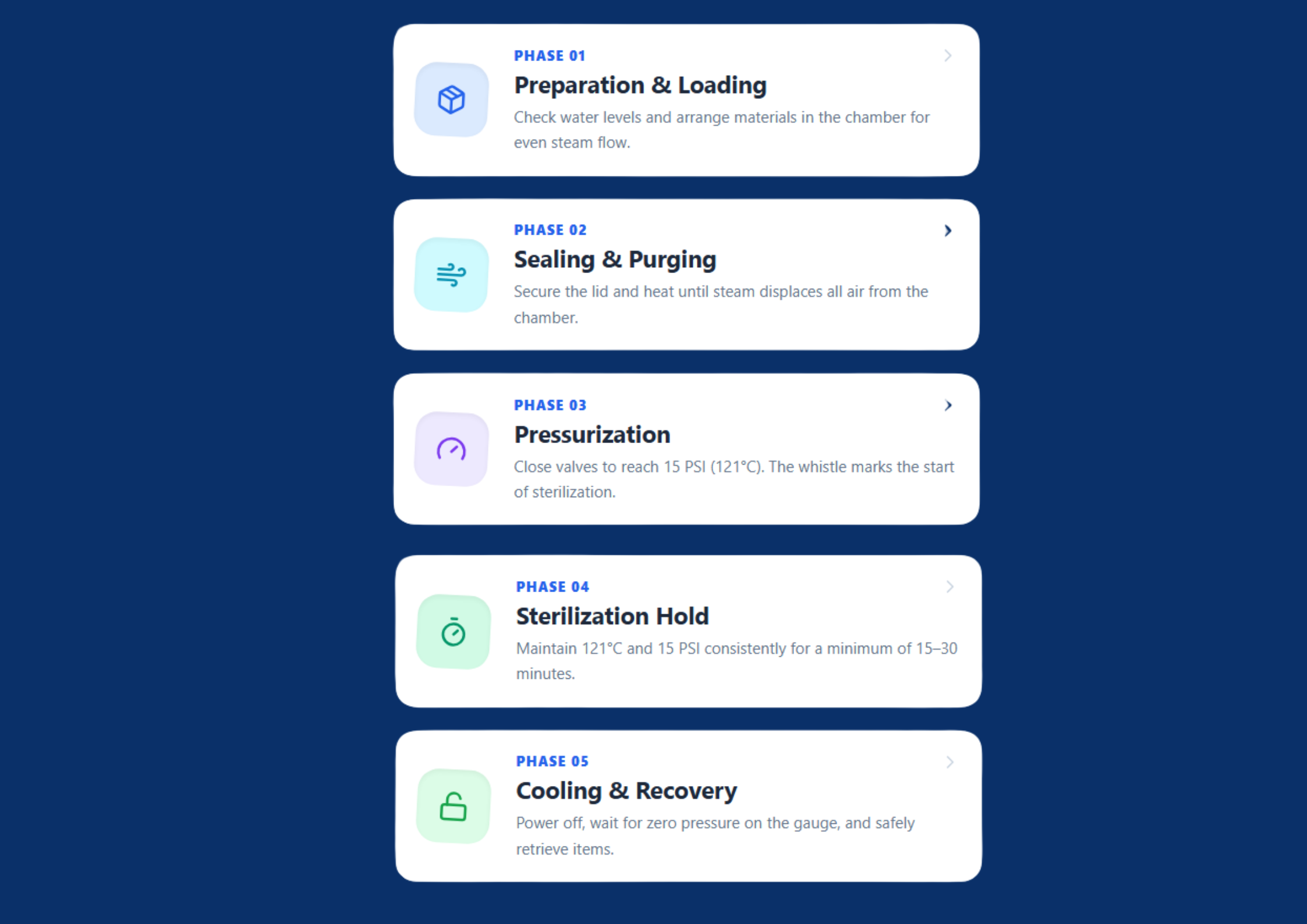
Steps of Autoclave Sterilization
Dry Heat
Dry heat sterilization is achieved by a hot air oven. This sterilization works with the principle of conduction of heat. This affects the microorganism by oxidizing the cellular constituents. The proper time and temperature for dry heat sterilization is 150°C (302 °F) for 150 minutes, 160°C (320°F) for 120 minutes or 170°C (340°F) for 60 minutes, and in the case of high velocity hot air sterilisers, 190°C (375°F) for 6 to 12 minutes.
Filtration
For filtration we typically use two types of filtrations, such as HEPA filters and Seitz membrane filters.
HEPA FILTERS
- It is a single sheet of borosilicate glass fiber that has been treated with a water-repellent binder.
- The filter, pleated to increase the overall surface area, is mounted inside a rigid, supportive frame.
- HEPA filters come in various shapes and sizes, from several square centimeters for vacuum cleaners to several square meters for biological containment hoods and room air systems.
- Control of airborne particulate materials with HEPA filters allows the construction of “clean rooms” and isolation rooms for quarantine, as well as specialized diagnostic/research laboratories.
- HEPA filters typically remove 0.3 μm test particles with an efficiency of at least 99.97%, including most microorganisms, from the airstream.
Membrane filters
- These are the most common type of filters used for liquid sterilization in the microbiology laboratory.
- Membrane filters are composed of high tensile strength polymers such as cellulose acetate, cellulose nitrate, or polysulfone.
- Membrane filters are prepared as circular membranes of about 150 μm thickness and contain millions of microscopic pores of uniform diameters, the size of which is adjusted based on requirements during the polymerization process.
- Porosities of membrane filters range from 0.1 μm to 10 μm and the most commonly used membrane filter has the pore size of 0.22 μm and 0.45 μm.
- The membranes are held in special holders and often preceded by depth filters made of glass fibers to remove larger particles that might clog the membrane filter. The solution is pulled or forced through the filter and is collected in previously sterilized containers.
Radiations
Radiation sterilization, or "Cold Sterilization," is a non-thermal method used to eliminate microbes from temperature-sensitive materials.
1. Ionizing Radiation (Gamma, X-Ray, E-Beam)
- Mechanism: Strips electrons to create reactive radicals (•OH, H•) that rupture DNA and degrade enzymes.
- Key Source: Cobalt-60 (Gamma rays).
- Best For: Bulk-packaged medical supplies (syringes, sutures) and food.
- Pros: High penetration through packaging; rapid and flexible.
- Cons: High cost; radioactive waste management; can damage certain plastics (PVC/PTFE).
- Control: Tested using Bacillus pumilus.
2. Non-Ionizing Radiation (UV, IR)
- Mechanism (UV): Forms pyrimidine dimers in DNA, preventing replication.
- Mechanism (IR): Kills via oxidation from generated heat.
- Best For: Disinfecting air, water, and surfaces (lab hoods, ORs, money).
- Pros: Effective at 260nm for germicidal action; safe for electronics.
- Cons: Zero penetration (blocked by glass, dirt, or paper); causes skin/eye damage.
Chemical Methods of Sterilization
Gaseous Sterilization
The fundamental mechanism of gaseous sterilization is alkylation (for EO and Formaldehyde) or oxidation (for Hydrogen Peroxide). These chemical agents interact with the microorganisms' cellular components:
- Target Molecules: Proteins, DNA, and RNA.
- Mechanism (Alkylation): The gas replaces hydrogen atoms in organic groups (such as amino, carboxyl, or hydroxyl groups) with alkyl groups. This causes the denaturation of enzymes and structural proteins.
- Mechanism (Oxidation): Agents like Hydrogen Peroxide generate free radicals (hydroxyl and hydroperoxyl) that broadly attack membrane proteins, lipids, and nucleic acids.
- Result: Disruption of these vital components leads to a halt in cellular functions and irreversible cell death.
Liquid Sterilization
This process involves submerging equipment in chemical sterilants to eliminate microorganisms and their spores. While generally reserved for low-contamination scenarios, it is essential for protecting delicate, temperature-sensitive medical tools.
- Hydrogen Peroxide An oxidant used in high concentrations (35–90%) for medical devices like endoscopes. Its greatest advantage is speed, with cycles as short as 28 minutes. However, it suffers from low material compatibility and poor penetration depth.
- Glutaraldehyde: A widely accepted agent that requires significant patience. Achieving full sterilization (including spore removal) can take up to 22 hours. Because it struggles to penetrate organic matter or tissue blocks, its use is typically limited to surface-level decontamination.
- Hypochlorite (Liquid Bleach): Commonly used as a disinfectant, bleach can act as a sterilant if items are submerged for 20–24 hours. It works by oxidizing organic compounds and denaturing microbial proteins. It remains a standard choice for cleaning workstations and managing biohazardous spills.
Applications in Veterinary Practices
- Sterilization of surgical equipment ensures that they are completely free of microbes before any animal surgery.
- It’s used in preparing laboratory media such as Petri dishes or test solutions, avoiding contamination.
- In animal care, it is used to sterilize feeding equipment, cages, and also protective gear that ensures a safe, germ-free environment for animals.
Advantages and Limitations of Each method
Choosing the Right Sterilization Method
- Based on material- Heat methods like autoclaving work well for metal or glass but can damage plastics or electronics.
- Based on microorganism resistance - Some bacterial spores are very tough hence demanding more aggressive methods such as ethylene oxide or prolonged heat. Hence, it is crucial to balance the material’s tolerance and the resilience of the microbes one needs to eliminate.
Conclusion
Sterilization is more than just a cleaning protocol; it is a fundamental aspect of modern medicine, food safety, and laboratory research. While disinfection might reduce the microbial load to safe levels, sterilization remains the only "absolute" in decontamination, ensuring a total absence of viable life forms, from the simplest bacteria to the most resilient spores.
As we have seen, no single method is a universal fix. The choice between the rapid, pressurized heat of an autoclave, the delicate precision of membrane filtration, or the deep penetration of gamma radiation depends entirely on the material at hand and the specific microbial threats involved.
By understanding these diverse methods, their mechanisms, strengths, and inherent limitations, professionals can maintain the highest standards of safety and efficacy. Whether in a high-stakes surgical suite or a food production facility, the goal remains the same: total microbial elimination to protect health and preserve life.


.jpg)





